Statement following the Board of Regents vote on July 22, 2021
July 22, 2021 | 4 p.m. PT
Today, the University of California Board of Regents approved an amended policy to govern affiliation agreements between UC and health care organizations that have policy-based restrictions on care. This action unequivocally states UC’s expectations that University personnel must be unencumbered in the provision of medically necessary care, even at non-UC sites that have policies against providing certain services.
University of California Health is focused on completing the implementation details that will guide its future agreements with covered organizations. These procedures will help ensure that UC clinicians at those facilities can provide evidence-based, medically-indicated care to all patients.
Additionally, the implementation steps will uphold the University’s commitment to transparency by creating mechanisms for reporting, review and audits of the covered affiliation agreements. The University will not enter into any new affiliation that fails to meet these requirements after July 1, 2021; any existing affiliation that does not meet these requirements must be amended to comply with this policy or phased out no later than December 31, 2023.
The two-year long process to achieve this final policy reflects many voices and perspectives. UC remains committed to delivering patient-centered, comprehensive medical care for all, while fighting discrimination and furthering health equity.
Statement following the Board of Regents vote on June 23, 2021
June 23, 2021 | 7 p.m. PT
Over the past two years, the University of California has worked diligently toward a resolution that expands Californians’ access to high-quality care and forcefully rejects all forms of discrimination. The action taken by the Board of Regents today (June 23) is an important milestone that clarifies shared aims and the University’s path forward.
The board endorsed key policy principles that emphasize the central role of human dignity in UC’s provision of health care. These critical stipulations strengthen the proposal originally offered and include the following requirements:
- Agreements with a covered organization must require the affiliate to offer care on a non-discriminatory basis;
- If transferring a patient to another facility for a procedure would be detrimental to the patient’s care in the clinical judgment of the UC clinician, the UC clinician at the covered entity must be permitted to provide any evidence-based, medically-indicated care; and,
- New affiliations cannot be entered into unless they comply with the new policy and any existing affiliations that do not comply must be phased out no later than December 31, 2023.
The action taken allows for a 60-day period to review and refine the implementation guidance. The intent of these refinements is to clarify that nothing not based on science and best medicine should interfere with the provision of care by UC personnel working at affiliated locations.
The constructive discussion today illustrated many of the complexities around finding a path forward on this challenging issue. The perspectives discussed, while varying in approach, reflect a shared commitment to fighting the pain of discrimination and finding additional ways to ensure UC continues to be a leader in providing the highest quality health care to everyone, regardless of location.
UC appreciates the many individuals who participated in this process and offered valuable input that informed the University’s actions. The heartfelt and passionate debate illustrates the complexity of the issues, the depth of emotion involved, and the imperative of ensuring UC clinicians can continue working with partners to provide high-quality care to as many Californians as possible.
Today’s decision by the Board of Regents affirms UC’s ongoing patient-centered approach to providing comprehensive medical care for all, fighting discrimination and furthering health equity.
UC Regents to Consider Policy at June 23 Meeting
June 17, 2021 | 5 p.m. PT
A special meeting of The Regents of the University of California and its committees is scheduled for Wednesday, June 23, 2021, by teleconference. The meeting will include consideration of a Regents Policy on Affiliations with Healthcare Organizations that Have Adopted Policy-Based Restrictions on Care. More information on the proposed policy can be seen here. Those wishing to participate in the public comment period, which is scheduled to begin at 9:30 am, can do so by following the instructions here.
University of California Health Report on Affiliation Impacts
March 23, 2021 | 5 p.m. PT

University of California Health conducted an assessment of the impact on patients and trainees if the University moved to end its affiliations with hospitals and health systems that have policy-based restrictions on care not based in federal law.
The analysis was in response to a request from the former president of UC and has continued and expanded under the current UC president after the transition in leadership.
By design, the report examines the issue from the perspective of UC patients, employees, retirees, students and their families who may lose access to UC providers who deliver care at non-UC host facilities. The work neither advocates for a particular course of action nor addresses all of the very challenging and complex issues involved.
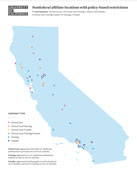
The University’s position is that all people deserve access to comprehensive medical care as a fundamental right. As the pandemic has demonstrated, clinicians and hospitals must be able to work together in the interest of public health for all Californians. We seek patient-centered solutions that eliminate discrimination, expand access to high-quality care and ensure personal health care decisions remain in the hands of patients and their physicians, based on evidence-based medicine and patient preferences.
The University continues to work with multiple parties to address concerns. While this work is underway, the University has already taken a number of steps. These include amending agreements with host facilities to assure that its personnel remain able, wherever they work or learn, to counsel patients on all medically appropriate options, to prescribe any needed medications, and to refer patients to facilities for procedures not available at the host location.
Frequently asked questions about UC affiliations
1. Why do you affiliate with health care organizations that have policy-based care restrictions not required by federal law?
UC has a range of affiliations, including many with federal and local public hospitals and health systems, the Veterans Administration Health System, and county and district hospitals. But these affiliations alone are insufficient to extend our services to many groups in need of our expertise and access to our clinical trials; or to supply sufficient opportunities for our health professions students to obtain the clinical opportunities they need.
Our physicians and medical students continue to help their patients navigate the steps necessary to receive the care they need despite the policy-based restrictions of these affiliates.
- UC physicians can advocate for transfer to another facility.
- In emergencies, UC physicians can even perform critical procedures that would normally be prohibited.
While the University strongly disagrees with these restrictions, and acknowledges it would be better for no patient or doctor to face these restrictions, they will exist regardless of whether UC is present. We must all continue to work together on eliminating these restrictions while also providing care to the greatest number of patients possible.
By having UC providers in these hospitals, we are putting the best providers in the nation into these affiliates, making medical decisions, not policy decisions. Hospitals with policy-based restrictions on care not required by federal law are often the only health care providers in the communities where they operate. This is true even in some urban communities, where these hospitals may serve patients most in need.
Additionally, UC must continue its work to train our next generation of doctors and health care providers. The University strives to train and graduate well-rounded, qualified health professionals who will thrive in any future work environment, and these hospitals provide much needed clinical sites for the rotations of our health professional trainees.
Affiliations with health systems also help the University further its research mission. When UC physicians see patients at other hospitals, they can facilitate those patients’ entry into clinical trials at UC. These clinical trials would otherwise not be available to the patients.
2. Why doesn’t UC just affiliate with other hospitals and systems that don’t have these kinds of limitations?
UC operates within the reality of California’s health care system that has a limited number of facilities and nearly 40 million residents. UC has a range of affiliations, including many with federal and local public hospitals and health systems, the Veterans Administration Health System, and county and district hospitals. The University also affiliates with other nonprofit and, in some cases, for-profit entities that do not have policy-based restrictions on care. However, in some locations even when these options are present, the facilities may not be open to affiliation. In some areas of the state, nonfederal health care systems with policy-based restrictions on care are the only ones with a presence or that are willing to serve vulnerable populations. These types of affiliations are necessary when a facility may offer a specialized capability or may be the only other hospital through which a UC presence can make certain services available. For example, only UCSF and Dignity Health answered this call when the City of San Francisco invited all of its hospitals to participate in a program to substantially increase access to adolescent mental health. Facilities with policy-based limitations on care not required by federal law also provide UC trainees the diversity of experience they need to be effective clinicians throughout their careers. Catholic-affiliated hospitals account for nearly one in six acute care U.S. hospital beds, and in some areas provide the only hospital care available.
3. How many patients would be affected if University of California Health stopped affiliating right now?
University of California Health clinicians provided services to more than 35,000 patients, with 77,150 unique patient encounters in fiscal year 2019 at nonfederal facilities that have policy-based care restrictions. Our focus on providing access and supporting the public health of Californians is part of our mission. We cannot leave these communities without care.
Patients primarily in rural California are accessing care from UC specialists with nearly 5,000 patients seen in FY 2019 for hematology/oncology; 3,800 seen for cardiology; 2,400 seen for pediatrics and more than 1,300 seen for neurology.
In addition, the current UC affiliations enable training for our nearly 15,000 health sciences students and trainees. In the Central Valley and Inland Empire, alternative options are limited. Without such affiliations, medical students and others might need to be redirected to metropolitan areas.
4. What is the University of California Health Report on Affiliation Impacts?
At the request of former UC President Janet Napolitano, University of California Health began a review to provide an analysis of the impacts of ending all existing agreements between UC’s academic health centers or health professional schools and organizations with policy-based restrictions on care. The requested review also included an analysis for the UC health benefits program of the potential impact that prohibiting affiliations with these types of health care providers would have on access to health care for UC employees, retirees, students, and their families covered by UC’s health plans. The resulting report evaluates the impact of a ban on affiliations with institutions that have policy-based limitations on care not required by federal law on 1) the number of patients across California who would lose access to UC expertise, 2) UC employees, retirees, and students who would lose access to non-UC hospitals, 3) the reduction in educational and training programs of our health professional schools, and 4) the financial impact on the University.
5. What were the key findings from University of California Health Report on Affiliation Impacts?
University of California Health found that a ban on UC affiliations with institutions that have policy-based limitations on care not required by federal law would hinder and often eliminate access to UC clinicians for tens of thousands of patients. Many patients would have limited access to both primary and specialty care, and in some cases, access to specialty care would be eliminated.
In fiscal year 2019, UC clinicians provided services to more than 35,000 patients, with 77,150 unique patient encounters whose access to those services at their local facilities would otherwise be terminated if these affiliations were to be prohibited. Patients who received care from a UC clinician at an affiliated facility that has policy-based limitations not required by federal law included those in need of cancer treatments, cardiology care and health care for children. Additionally, patients served through these affiliations come from some of our most vulnerable communities.
The financial analysis of these activities shows a modest benefit from these affiliations but constitutes only a small portion of the University of California Health system revenue. UCH is a $13B enterprise that realized $20M in net revenue in fiscal year 2019 from these professional services agreements or less than 0.2 percent of our system’s overall net revenue. Our focus on providing access and supporting the public health of Californians is part of our mission. Our system is one of the largest providers of care to Medi-Cal patients despite representing less than six percent of the non-federal, short-term, acute care hospital beds in California (https://www.ahd.com/states/hospital_CA.html).
The affiliation impact report is available online at https://www.universityofcalifornia.edu/sites/default/files/UCH-report-on-affiliation-impacts-may-2020-final.pdf.
UC comment on proposed legislation
February 10, 2021 | 11 p.m. PT
On February 10, the University of California learned of state legislation that would prohibit physicians and other clinical personnel, and trainees from UC’s academic health centers from providing patient care at facilities with policy-based restrictions on care.
We are carefully examining the implications of the bill including its impact on core areas of the University’s designated responsibilities. We strive to promote practices that maximize equitable access to health care, and agree strongly that all Californians should have access to comprehensive services without interference.
We look forward to working with the Legislature, health professionals and other key community stakeholders to meet our shared goals of access, quality and non-discrimination.
Community Update – Recommendations Expected Late This Year
June 30, 2020 | 2 p.m. PT
The University is continuing to assess how it can best meet the clinical care needs of the people of California while ensuring that all patients seen by UC clinicians at any site retain access to comprehensive health services.
UC expects all of its clinical personnel and trainees, wherever they work or learn, to make decisions consistent with the standard of care and their independent professional judgment, respecting the needs and wishes of each individual patient; counsel patients about all medically appropriate treatment options; prescribe any needed interventions; and transfer or refer patients to other facilities when the care they need is not available where they are being seen.
Contracts that had included inappropriate language have been or are being amended to remove any requirement that UC or its clinical personnel should comply with policy-based restrictions on care.
We expect to have completed the work this summer. We expect that recommendations will be presented to the Regents late this year.
More information will be posted online as soon as the timing of that meeting is finalized.
Update on the presentation of the Chair's Report
April 29, 2020 | 11 a.m. PT
Due to the COVID-19 pandemic, the presentation of the Chair’s Report from the Working Group on Comprehensive Access (WGCA) will be postponed. We will announce the new date here once it is scheduled.
Online Public Comment Period Ends
Chair’s report to be discussed at Regents in May
February 21, 2020 | 5 p.m. PT
The online public comment period has ended for the Working Group on Comprehensive Access (WGCA) Chair’s Report. The University thanks everyone who took the time to provide feedback on this important issue. More than 4,500 public comments were submitted from January 28 through February 21, 2020.
The Chair’s report outlines two potential paths for the University’s consideration as it examines affiliations between its academic health systems and non-UC medical facilities, particularly those that have policy-based restrictions on certain types of health care.
Public comments to date will be reviewed along with additional information that President Janet Napolitano requested from UC Health. No decisions have been made. The Chair’s report will be discussed at the May meeting of the Board of Regents.
The Chair’s report and associated correspondence remain available below for review.
Letters sent to the University after February 21 will continue to be accepted consistent with University practice, but submissions received after March 16 may not be included in the analysis and input process.
Please be aware that correspondence may be read or answered by members of President Napolitano's staff or appropriate campus personnel. Please also note that the Office of the President retains copies of all correspondence sent to the president, and that all correspondence is considered a matter of public record and is, therefore, subject to disclosure under the California Public Records Act.
Download the WGCA report and appended documents (PDF)
WGCA Chair’s Report Available for Review
Public Comment Period Runs Through February 21, 2020
January 28, 2020 | 10 a.m. PT
In August of 2019, President Napolitano convened a Working Group on Comprehensive Access (WGCA) comprised of academic and health leaders from across the University. The WGCA was provided 90 days to develop recommendations that “would ensure UC’s values are upheld when its academic health systems collaborate with other health systems” and “to ensure that UC personnel will remain free, without restriction, to advise patients about all treatment options and that patients will have access to comprehensive services.”
The WGCA met six times during the fall of 2019. The members reviewed a wide range of materials, perspectives and arguments.
While there was important agreement on many issues, the working group did not reach consensus on the central question of whether UC should have affiliations with health care organizations that have institutional policies limiting the services provided at their facilities. Examples of such institutional policies include prohibitions on the use of contraception, abortion, assisted reproductive technology, gender-affirming care for transgender people, and the full range of end-of-life options.
The University has affiliations with a wide range of non-UC medical facilities to help fulfill its public service mission of providing care to all Californians and to provide additional training sites for rotations of health professional students who need field experience in various settings.
The WGCA held its last meeting in mid-December. In late December, the Chair of the WGCA prepared a report that attempted to summarize the viewpoints of WGCA members and outlined the two options discussed by WGCA committee members. One path would prohibit patient care and training agreements with institutions that have policy limitations on care, while the other path would allow such affiliations but only if certain protections, monitoring and compliance protocols are put in place. The report was transmitted to the president in late December for her consideration.
Although the work of the WGCA and submission of the Chair’s report are significant milestones, they are not the end of the process.
Today, the University published the Chair’s report and associated correspondence and initiated a public comment period that will continue through February 21, 2020. View the report and access the feedback mechanism at ucal.us/wgca.
The report will also be presented to the Board of Regents at its May 2020 meeting.
Progress Update: Public Comment Period to Begin Later This Month
January 7, 2020 | 10 a.m. PT
The Working Group on Comprehensive Access (WGCA) has completed its deliberations. The WGCA is one of three action steps announced by the University in August to address concerns about certain agreements with non-UC medical facilities, including faith-based hospitals.
UC President Janet Napolitano would like to thank members of the working group, who spent considerable time and effort examining a complicated and important set of issues. The chair’s report is now with the president, who will consider it along with additional input from employees, regents and the public over the coming months.
Later this month, the University will make the report available to the public along with an online mechanism for comment. Current plans call for a presentation and discussion of the report at the May 2020 meeting of the Board of Regents.
UC is committed to thoughtfully considering its future policies and practices around affiliations with non-UC medical facilities. UC seeks to contribute meaningfully to an ongoing national dialogue about how and when public entities form affiliations with outside organizations that may have both shared and differing values.
The just-completed report is an important step, but it is not the end of the input or consideration process.
A Progress Update: UC Addresses Concerns with Health Service Agreements
November 15, 2019 | 10 a.m. PT
The University of California is providing this update on efforts to address concerns about its agreements with non-UC medical facilities, including faith-based healthcare facilities.
The University recognizes the broad set of complex issues involved. Earlier this year, UC Health began to take steps to ensure its expectations are clearly articulated in these agreements and understood by UC personnel working off-site at non-UC medical facilities. These affiliations allow the University to remain focused on increasing access to care for medically vulnerable or underserved patients who seek care at community clinics and community hospitals. Services include oncology, care for stroke and cardiovascular conditions, neonatal intensive care and mental health, all of which are enhanced through the expertise of UC clinicians at these facilities.
The action steps taken to date include:
- Pursuing amendments to certain existing contracts to revise language that may be inconsistent with UC values and expectations. Thus far, several dozen agreements are in the process of being updated and more such revisions are expected to follow.
- Implementing interim guidelines for agreements under which our providers and trainees work with other health systems until longer-term guiding principles and compliance measures have been adopted. These guidelines are in place.
- Convening the Working Group on Comprehensive Access (WGCA), a multidisciplinary group of academic and health system leaders to evaluate current practices and provide recommendations to ensure UC values are upheld in affiliations with other health care organizations.
The WGCA will submit its report and recommendations to President Napolitano by the end of this year as part of a continuing process. After carefully evaluating the report and consulting with the UC Board of Regents and others, the president may also request additional information or input, initiate steps necessary to formalize some of the recommendations or pursue a variety of other options.
Given the complexity of this issue, a large number of stakeholders involved and the potential implications for patient care, teaching and research, UC is approaching this issue in a careful, deliberative manner that respects a variety of perspectives.
While this process continues, the University wants to reassure the public that UC personnel who are working or training at non-UC facilities will make clinical decisions consistent with the highest standards of care and their independent professional judgment, which considers the needs and wishes of each patient. This includes informing patients of all of their health care options, whether or not a particular option is available at the site where they are being seen; prescribing any interventions that are medically necessary and appropriate, whether or not dispensed at that site; and referring patients to other facilities when the care such patients need is not available where they are being seen.
UC President Convenes Group to Develop Recommendations Regarding Terms of Agreements with Other Health Systems
August 2, 2019 | 10 a.m. PT
University of California President Janet Napolitano today announced the launch of a working group to ensure that UC’s values are upheld when its academic health systems collaborate with other health systems.
The Working Group on Comprehensive Access (WGCA) will review common types of health system agreements where patient access to care might be limited due to policy restrictions on services provided, and provide written recommendations to guide future collaborations. The intent is to ensure patients under the care of UC personnel at non-UC facilities have access to a full range of health care services.
The University of California’s health enterprise includes six health systems and 18 health professional programs. UC’s clinical expertise is often sought out by other health care organizations to strengthen or augment clinical capabilities, and UC physicians often provide services at non-UC facilities. UC also operates the largest training program in the state for health professionals. UC’s medical, nursing, pharmacy and public health students, residents, and other trainees broaden their educational and field experience by rotating through a variety of settings, including non-UC facilities.
The WGCA is an outgrowth of recent public debate about the University’s ability to ensure patients receiving care from UC personnel at non-UC facilities retain access to a comprehensive range of clinical services. The University withdrew from negotiations to expand its relationship with another health system earlier this year after concerns were raised that UC had not provided sufficient assurance of non-interference in access to care.
“The vigorous debate around that proposed agreement demonstrated we must do more to ensure UC’s values are embedded in all of our collaborative efforts and to address the concerns that were raised,” said UC President Janet Napolitano. “Our expectation has always been that UC health professionals provide UC-level expertise to all patients, including at health facilities operated by other organizations.”
Affiliations and other health services and training agreements allow UC to serve patients at facilities that are best suited to their care requirements or their geographic location. UC’s medical centers are often full, and agreements enabling UC providers to care for patients at non-UC hospitals and clinics allow more patients to receive UC’s high quality medical care. Additionally, hospitals in underserved areas have difficulty recruiting certain types of providers. Agreements for UC physicians to care for patients in non-UC facilities increase the number of access points in a community, which is important to fulfill the University’s service mission. However, this expanded access must be accompanied by clear expectations that preserve physician autonomy and allow patients to evaluate and choose from all appropriate care options.
The WGCA includes leadership from campuses, medical centers, and the University’s Academic Senate and will consider a broad array of collaboration scenarios – encompassing respect for a diversity of opinions. The group will review concerns raised about patient access in other health systems, as well as UC’s operational, training and patient care needs. The group’s main charge is to develop written recommendations for consideration by President Napolitano regarding the terms under which UC academic health systems will enter into affiliations with other health systems to protect patient access to comprehensive care. The Working Group’s written preliminary recommendations are expected in the fall.
UC has a long-standing expectation that its physicians will remain free to counsel patients about all treatment options, and that patients will have access to comprehensive services. However, the language used in some agreements with other health systems may appear to contradict these expectations. As such, and in parallel to the forward-looking efforts of the Working Group, the University is seeking to amend current agreements to clarify expectations of UC trainees and health professionals when providing care at non-UC health facilities. Additionally, the University has developed interim guidelines that will govern new agreements and renewals of expiring contracts deemed critical to UC's clinical and academic missions.
About UC Health
The University of California’s health enterprise, UC Health, includes six academic medical systems, health professional schools in medicine, nursing, dentistry, optometry, pharmacy, public health and veterinary medicine, clinical oversight of student health and counseling centers, and oversight of self-funded health plans offered to UC employees.