Elizabeth Fernandez, UC San Francisco
To address the growing problem of people being overdiagnosed and overtreated for cancer, a group of scientists convened by the National Cancer Institute and chaired by a UC San Francisco breast cancer expert is proposing a major update of the way the nation approaches diseases now classified as “cancer.”

The “Viewpoint” article was published online on July 29 in the Journal of the American Medical Association.
When cancer screening programs were widely initiated three decades ago, medical knowledge of the disease was more simplistic. The intent was to detect cancer at its earliest stages to reduce illness and mortality, but in fact early diagnosis has not led to a proportional decline in serious disease and death, the scientists write in the JAMA commentary.
Instead, screening programs are identifying not only malignant cancers, but also slow-growing, low-risk lesions, and sweeping them into the same treatment process. As a result, patients are being diagnosed and treated for forms of cancer that might never actually harm them – a phenomenon that’s been termed overdiagnosis, which translates to “too much medicine.”
Now, with the advancement of scientific understanding of the biology of cancer, the authors say it is time for significant changes in practice and policy.
Not just one disease
“By recognizing that cancer is not one disease, but a number of different diseases, we can individualize our treatment based on biology and avoid overtreatment,” said panel chair Laura J. Esserman, M.D., MBA, director of the Carol Franc Buck Breast Care Center at the UCSF Helen Diller Family Comprehensive Cancer Center.
The authors recommend creation of a new classification for tumors that are indolent (unlikely to cause patients harm). For example, ductal carcinoma of the breast — currently considered the earliest form of breast cancer — would no longer be called cancer. The authors also call for the formation of registries for lesions with low potential for malignancy, and for a multidisciplinary approach across pathology, imaging, surgery and other medical specialties “to revise the taxonomy of lesions now called cancer.”
The key, they say, is to improve screening strategies to avoid overtreating tumors that would not be lethal, or that would not even have come to medical attention.
The JAMA article is comprised of recommendations from a working group formed last year during a meeting convened by the National Cancer Institute. The group was charged with developing a strategy to improve current approaches to cancer screening and prevention.
"Although our understanding of the biology of cancer has changed dramatically, perceptions on the part of the public, and among many physicians, have not yet changed,” Esserman said. “Cancer is still widely perceived as a diagnosis with lethal consequences if left untreated.”
The commentary was co-written by Ian M. Thompson, M.D., professor at the University of Texas Health Science Center at San Antonio; and Brian Reid, MD, PhD, director of the Seattle Barrett’s Esophagus Program and member of the Human Biology Division at the Fred Hutchison Cancer Research Center in Seattle. The three authors served as chairs of the NCI working group.
An internationally known leader in the field of breast cancer, Esserman, a UCSF professor of surgery and radiology, is leading an effort to change the delivery of breast cancer services and the information systems used to support both research and patient care.
Overdiagnosis occurs across many medical conditions
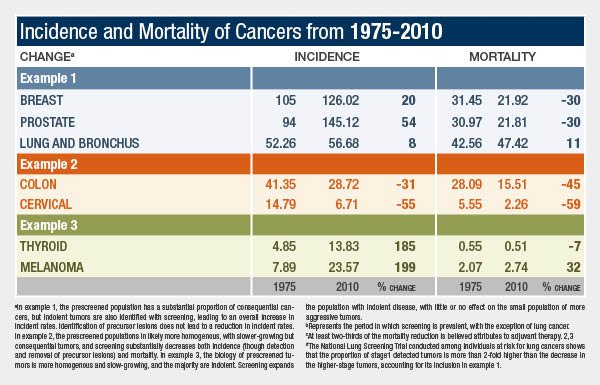
Overdiagnosis is occurring across many medical conditions, but is particularly common in breast cancer, lung cancer, prostate, thyroid cancer and melanoma, said the authors.
They cite DCIS, or ductal carcinoma of the breast, and Barrett’s esophagus as illustrations of how the detection and surgical removal of what have been called precancerous lesions have failed to lead to lower rates of invasive cancer.
By contrast, the authors said, colon and cervical cancer serve as examples of “effective screening programs in which early detection and removal of precancerous lesions have reduced incidence as well as late-stage disease.”
Cancer screening should have three important missions, the authors write: To detect disease that would ultimately harm the patient; to uncover tumors that benefit from intervention; and to detect disease that is more likely to be cured or better treated when spotted early.
Optimal screening frequency depends on a cancer’s growth rate. If a cancer is fast growing, screening is less likely to be effective. “If a cancer is slow growing but progressive, with a long latency and a precancerous lesion, screening is ideal and less frequent screening (e.g., 10 years for colonoscopy) may be effective,” the authors said.
The recommendations include:
- Recognize that screening will identify indolent cancers.
- Change terminology and omit the word “cancer” from premalignant/indolent conditions;
- Convene a multidisciplinary body to revise the current taxonomy of cancer and to create reclassification criteria for indolent conditions;
- Create observational registries for lesions with low potential for malignancy — generate the data to provide patients and their doctors “with confidence to select less invasive interventions;”
- Develop, validate and adopt molecular diagnostic tools that identify indolent or low-risk lesions;
- Mitigate overdiagnosis: appropriately reduce frequency of screening exams while focusing on high-risk populations, and raise the threshold for patients being recalled for re-testing and biopsy.
“Although no physician has the intention to overtreat or overdiagnose cancer, screening and patient awareness have increased the chance of identifying a spectrum of cancers, some of which are not life threatening,” the authors wrote. “The ultimate goal is to preferentially detect consequential cancer while avoiding detection of inconsequential disease.”