Kim McDonald, UC San Diego
An international team of scientists headed by biologists at UC San Diego has discovered that an important class of stem cells known as human “induced pluripotent stem cells,” or iPSCs, which are derived from an individual’s own cells, can be differentiated into various types of functional cells with different fates of immune rejection.
The scientists also found that these cells may not be rejected by the immune system if iPSCs are turned into retinal pigment epithelium cells destined for the eye.
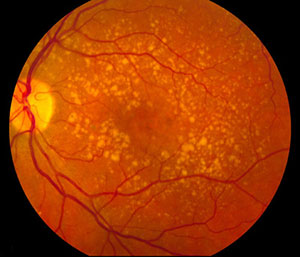
Credit: National Eye Institute, National Institutes of Health
Their discovery provides hope for the development of human stem cell therapies to treat macular degeneration, a major cause of blindness and visual impairment in older adults. An estimated 30 million to 50 million people worldwide are affected by the degenerative medical condition.
The achievement was published in a paper in this week’s early online edition of the journal Cell Stem Cell, which will again appear in the Sept. 3 issue of the print journal.
The research effort was headed by Yang Xu, a biology professor at UC San Diego who discovered with colleagues in 2011 that even though iPSCs are derived from an individual’s own cells, the abnormal gene expression can cause the immune system to reject certain cells derived from iPSCs.
That could have been a major impediment to the safe use of iPSCs, which are regarded as particularly attractive candidates for stem cell therapies because they can be differentiated into a wide variety of cell types, are not derived from embryonic tissue and are not subject to restrictions that limit the use of human embryonic stem cells.
Funded by a $5.12 million grant from the California Institute for Regenerative Medicine, the state’s stem cell agency, Xu and his colleagues at UC San Diego earlier developed “humanized” laboratory mice with a functional human immune system capable of mounting a vigorous immune rejection of foreign cells derived human embryonic stem cells.
“Human and mouse immune systems are quite different,” explained Xu, “so we developed a humanized laboratory mouse that carries a functional human immune system. This provides a unique opportunity to evaluate the human immune responses to stem cells.”
In their experiments, the researchers developed a variety of cell types from human iPSCs, then tested the immune responses in humanized mice with the immune system of the same individual. They discovered that smooth muscle cells were highly “immunogenic,” or strongly rejected by the immune systems of the humanized mice, while retinal pigment epithelial cells were tolerated by the immune system, even when transplanted in parts of the body that provide the environment for robust immune rejection.
The researchers showed that the abnormal expression of immunogenic antigens in smooth muscle cells, but not in retinal pigment epithelium cells, contributes to the differential immunogenicity.
“Immune rejection is a major challenge for stem cell therapy,” Xu said. “Our finding of the lack of immune rejection of human iPSC-derived retinal pigment epithelium cells supports the feasibility of using these cells for treating macular degeneration. However, the inflammatory environment associated with macular degeneration could be an additional hurdle to be overcome for the stem cell therapy to be successful.”
The research team included UC San Diego scientists Tongbiao Zhao, Zhen-ning Zhang, Dilyana Todorova, Meiyan Wang, Jingjin He and Kun Zhang; Peter Westenskow and Martin Friedlander of The Scripps Research Institute and colleagues from Columbia University, UC Santa Barbara, Chinese Academy of Sciences, Southern Medical University, Jilin University and Guangzhou University of Traditional Chinese Medicine.
The study was funded by grants from the California Institute for Regenerative Medicine, National Eye Institute of the National Institutes of Health (EY11254), Chinese Academy of Sciences, Chinese Ministry of Science and Technology and the National Natural Science Foundation of China.