Nina Bai, UC San Francisco

Editor’s Note: This story was updated on Jan 31. by UCSF to reflect new information about the number of cases worldwide and that the virus can be transmitted by asymptomatic persons. On Feb. 11, it was updated to include the new name, COVID-19, granted by the World Health Organization.
A new coronavirus, related to the SARS and MERS diseases that have caused epidemics, has been discovered in China and started to spread.
Just weeks since the viral illness was first reported in Wuhan, China, health experts globally are working on containing and treating it. As of Jan. 31, it has killed over 250 people and sickened more than 11,000. Cases have now been reported in Asia, Australia, Europe and North America, including seven cases in the United States. Johns Hopkins University has a real-time map of confirmed cases.
To put the latest news in context, we asked UC San Francisco infectious disease expert Charles Chiu, M.D., Ph.D., about the origins of the Wuhan virus and public health risks going forward.

Credit: UCSF
What do we know about the mysterious new virus that appeared in Wuhan?
This is a new virus. The initial cases came from the city of Wuhan in association with exposure to a seafood market.
The virus has been identified, cultured and sequenced. In fact, there are now 24 complete genomes of the virus, which are publicly available. And what the genome analysis suggests is that this is a relative of the SARS and MERS coronaviruses as well as other known human coronaviruses.
What is a coronavirus?
Coronavirus is a family of viruses that causes the common cold, but the spectrum of disease can range from the common cold to severe life-threatening pneumonia. They’re named for the spike proteins on the surface of the virus that make the virus look like a crown or star.
There are seven coronaviruses that are known to infect humans. The emergence of two of these coronaviruses, SARS in 2002 and MERS in 2012, occurred as a result of animal-to-human, or zoonotic, transmission events. The same is likely true for the new coronavirus from Wuhan, which has been officially named COVID-19 (formally designated 2019-nCoV) by the World Health Organization. SARS, MERS, and COVID-19 are all associated with human-to-human transmission.
How dangerous is the new virus?
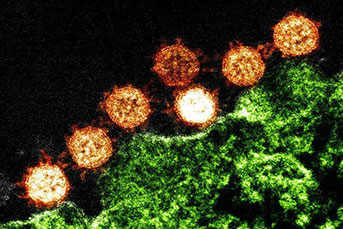
Credit: National Institutes of Health
There are two key questions we need to address before we can really understand how widely this virus is going to spread and how much of a threat it poses.
The first question is what’s the animal reservoir for the virus? Nearly all coronaviruses are thought to originate from bats, and the genome sequence of COVID-19 is 96 percent identical to the sequence of a bat coronavirus. However, bat-to-human transmission is thought to be exceedingly unlikely. The zoonotic “jump” from animals to human usually occurs through an intermediate animal reservoir. In the case of SARS, it was the civet, which was a cat-like animal that was used for consumption in the animal markets in China. With MERS, it was camels.
Coronaviruses in general are thought to be transmitted through respiratory droplets, contact with infected secretions, and fecal-oral transmission — you don’t necessarily have to eat an infected animal, and the infected animal can be asymptomatic.
The other key question is the efficiency of human-to-human transmission. SARS is more efficient at spreading from person-to-person than MERS, for example.
Right now, we don’t know the transmission efficiency for the new virus. A case was reported from China where one patient apparently infected 14 health care workers at the hospital, and it’s possible that some patients, known as super spreaders, are more infectious than others. We don’t know whether that particular patient was a super spreader or whether this reflects the fact that this virus is already very efficient at human-to-human transmission.
Until we know, we have to make the assumption that this is a virus that spreads quite efficiently, which is why there are now mandatory screenings at airports and enhanced monitoring in local hospitals here for possible cases of COVID-19 infection.
Reports in the New England of Journal of Medicine and The Lancet have shown that asymptomatic transmission is possible from person to person, making the virus more difficult to eradicate.
Will this virus mutate?
The virus has already likely mutated to acquire the capacity to “jump” from animals to humans and to be transmitted person-to-person. Since this is an RNA virus, it will continue to mutate as long as it continues to circulate in humans. Additional mutations as the virus adapts to the human host may make the virus less severe or more severe, or less or more efficient in spreading. It’s too early to tell what will happen, which is why ongoing surveillance by sequencing virus genomes is so important.
Are there tests to screen for the new virus?
This virus is different enough that the common coronavirus tests used clinically cannot detect it, meaning that new and accurate diagnostic tests to detect this virus are urgently needed. The Centers for Disease Control and Prevention (CDC) has a PCR (polymerase chain reaction) laboratory test for specifically detecting this virus that can be done in four hours, and plans are to rapidly disseminate this test to state and local public health laboratories.
Just two weeks ago we published a paper in Nature Microbiology on a metagenomic sequencing technique that enables you to rapidly identify virtually every RNA viral pathogen, including Zika virus, West Nile virus, Ebola virus, Marburg, Lassa, yellow fever, influenza, any virus. We are currently adding COVID-19 to our list of viruses that we can detect. It’s quite rapid — the entire procedure can be done under six hours.
We are seeking to work with public health laboratories in California to deploy this metagenomic sequencing test for monitoring COVID-19 and sequencing the genome of any cases that are identified.
What are the signs of having this coronavirus infection?
Based on the reports, the symptoms of respiratory infection from COVID-19 are very similar to those from other coronaviruses: nasal congestion, headache, cough, sore throat and a fever. In some patients, these symptoms can worsen into pneumonia, with chest tightness, chest pain, and shortness of breath. If you’re elderly, immunocompromised, or if you have other comorbidities such as heart disease, liver disease, you are at higher risk of developing severe pneumonia and dying from the disease.
How long would it take for symptoms to appear after infection?
Again, we don’t really know about the incubation period for this virus, but I can tell you that for coronaviruses in general, the incubation period is thought to be two to 10 days, with a median period of five days. The incubation period is extremely unlikely to be longer than two weeks.
So it sounds like there are still many unknowns about this virus.
That’s correct, I would like to stress that there’s a lot about this virus we don’t know at this point in the outbreak.
However, we do know that there’s very little diversity in the genome sequence. The 24 viral genomes that have been sequenced, some from China, others from Japan and Thailand, are nearly identical. What that means is that the actual zoonotic animal-to-human transmission event occurred very recently, and that China may have detected it very early in the course of the outbreak.
We also know that there are documented cases of human-to-human transmission as shown by the hospital-acquired cases, and evidence of sustained cycles of transmission, as evidenced by secondary infections in household members who were not exposed to the markets from which the initial cases originated. We also know that there have been deaths from this virus, the majority in older men with underlying health problems, but also in a healthy young man. So it’s definitely something to worry about.