Milenko Martinovich, UCSF

Every other Tuesday morning, a team of UCSF nursing students arrives near the main branch of the San Francisco Public Library, medical supplies in tow. For the next few hours, they’ll provide nursing advice and lend a compassionate ear to people experiencing homelessness in San Francisco.
The nurses know they can’t solve San Francisco’s homelessness crisis a few hours a day every other week, but that’s not their primary goal. Their objective is simple: There are people in need, and they have the skills and expertise to help.
The nurses’ dedication has not only made an impact on the city’s streets, but also at the School of Nursing where “Street Nursing” is on a path to becoming an elective. From the streets, to the classroom, to faculty-led research, the School’s faculty and students are striving to tackle the needs of people experiencing homelessness.
Delivering “bridge care”
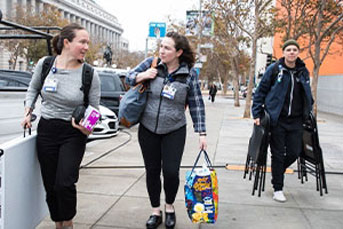
Credit: UCSF
From their perch on Fulton Street in the city's Civic Center, the students who make up the Street Nursing team provide “bridge care,” considering many people experiencing homelessness do not want to visit a hospital or clinic. Advising someone how to keep a wound from getting infected and avoid an emergency room visit is a victory.
As “nursing ambassadors,” the team helps alleviate clients’ reluctance about seeking medical care when it’s necessary.
“A lot of what we’re doing is referring clients to primary care and to other preventive services, so they don’t get too acute,” said student Janelle Silvis. “We talk with the client and figure out what works best for them. We build rapport with clients by letting them know we care about them and that they can be honest about their health problems.”
The students have had more than 200 encounters with people experiencing homelessness since April. Some are marginally housed while others are unsheltered. They range in age from early 20s to 60s and 70s. Some are in relatively good health considering their housing situations; others are not.
Due to liability concerns, the team does more consulting than treating. For instance, they don’t treat wounds. They inspect them, and offer advice and basic supplies on how to care for them.
“We do a lot of listening,” said student Tessa Rubin.
Most of the team’s medical supplies are bought out of their own pockets. The team is seeking other sources of funding and accepts in-kind gifts.

Credit: UCSF
The Street Nursing members, who began in the School’s Master’s Entry Program in Nursing (MEPN), have previous experience with this type of outreach: Taylor Cuffaro and Silvis worked with the San Francisco AIDS Foundation and participated in syringe access services; Megan Grant worked with an RV clinic, treating those in need on the streets of Chicago; Katie Machado is co-director of the leadership board for the UCSF Shelter Clinic; and Rubin worked at the Homeless Services Center in Santa Cruz and the Mission Neighborhood Resource Center in San Francisco. Alumna Michaela Lambert, who co-founded the team, participated in a youth HIV prevention program in Washington, D.C., and also worked at the Shelter Clinic.
“We have all this experience with homelessness,” Grant said. “How can we be useful? How can we put our nursing skills to work? Doing something feels better than doing nothing.”
They partnered with Lava Mae, a San Francisco-based nonprofit that provides mobile showers and toilets for people experiencing homelessness. The team sets up shop near the showers, and visits with those who come to them for advice.
Rubin said the nurses asked themselves some difficult questions before beginning this work.
“I think it’s important anytime you enter a community to ask, ‘are we the right people to do this work?’” she said. “We really paused to take stock of that. We regularly hear how happy and grateful people are that we’re out there. I think we’ve proven there is a need for the service we’re providing.”
Becoming an elective

Credit: UCSF
The path to a potential elective began last spring when the team hosted a study group. They expected 30 nursing students, but 60 showed up. Encouraged by the turnout, they enlisted Heather Leutwyler, associate professor in the Department of Physiological Nursing, to help navigate the course approval process.
“They have a vision for what they want to do,” said Leutwyler, whose research and clinical experience deals with homelessness. “I’m trying to step in and help them where I can, but also stay out of their way.”
The course, which could begin in Spring 2020, would contain lectures on topics including common dermatological conditions, foot care concerns, and wound care for people who are experiencing homelessness as well as learning activities — like many UCSF nursing courses. But this course will be student-run. The team will secure expert guest lecturers and lead the learning activities.
The plan is for the leadership duties to pass to new students who join the Street Nursing team, with Leutwyler and assistant adjunct professor Shannon Smith-Bernardin providing support.
The course is currently being reviewed by the School’s Master’s Program Council.
Analyzing homelessness through research
While the Street Nursing team embodies outreach, the School’s Homelessness Workgroup represents its research component.
The group was created by Leutwyler, who became increasingly frustrated with the homelessness crisis and how it affects patients in her practice and research studies. A Q&A on the UCSF Department of Psychiatry’s attempt to attack the homelessness problem, inspired her to do something similar at the School.
“We have all these great faculty that are doing all this great work,” Leutwyler said. “Why don’t I get them together and see if we can come up with an idea?”
Members of the work group have already been researching various angles of homelessness and policy initiatives to support housing for low-income adults, families and the elderly. For example, Leslie Dubbin, assistant professor in the Department of Social Behavioral Sciences, studies the health and social impacts of public housing renovation financed through the Rental Assistance Demonstration Program — a federal program that relies on public-private partnerships to renovate public housing units long in need of vast capital improvements.

Credit: UCSF
A second study explores the impacts of HOPE SF, a neighborhood redevelopment initiative that demolishes four of the largest and most distressed public housing projects in San Francisco, and transforms them into mixed-income communities. Using a mixed method approach (ethnography and analysis of 10 years worth of clinical medical record data obtained from two of the largest health service systems in San Francisco), the goal of these studies is to assess the health status of public housing residents before, during and after renovation and/or redevelopment as well as residents’ experiences living through them. Through these studies, a better understanding of the linkages between health, housing quality and community may be gained.
Smith-Bernardin has experience with street outreach in Los Angeles and Alameda County, and has been integral in the growth of sobering centers, which are facilities designed to treat non-emergency events involving alcohol. Smith-Bernardin has cited research that indicates up to 40 percent of people transported to emergency departments via ambulance are intoxicated.

Credit: UCSF
Smith-Bernardin, a co-founder of the National Sobering Collaborative, said an important factor to keep in mind when dealing with individuals experiencing homelessness is that many of them are victims of trauma such as child abuse, veterans battling post-traumatic stress disorder, and those whose family members have been the victims of violence.
“You have to have the approach that there’s a lot more going on than someone not paying their bills or not taking their meds,” she said.
The Homelessness Workgroup’s goal is to develop a new research project and get it funded, Leutwyler said. Initial discussions have focused on examining the “lived experience of homelessness” — what this population endures on a daily basis and how nurses can positively affect the situation.
Said Leutwyler: “How can we prevent people from losing their housing? How can we help people when they get housing to maintain it? If they are experiencing homelessness, how can we help them manage the experience better? Or better yet, help them secure housing. There’s a lot of excitement from looking at the patient perspective and where can nursing make an impact.”

