Jess Berthold, UCSF
Joe Bojanowski, 56, has had exactly one colonoscopy – and, not surprisingly, it made him grateful he hasn’t needed more.
If he’d been diagnosed with inflammatory bowel disease (IBD) much earlier than summer 2022, odds are high that he’d have had several by now. The condition, marked by frequent diarrhea, abdominal pain, fatigue and weight loss, requires doctors to keep tabs on the bowel — and until recently, that would have meant repeat colonoscopies.
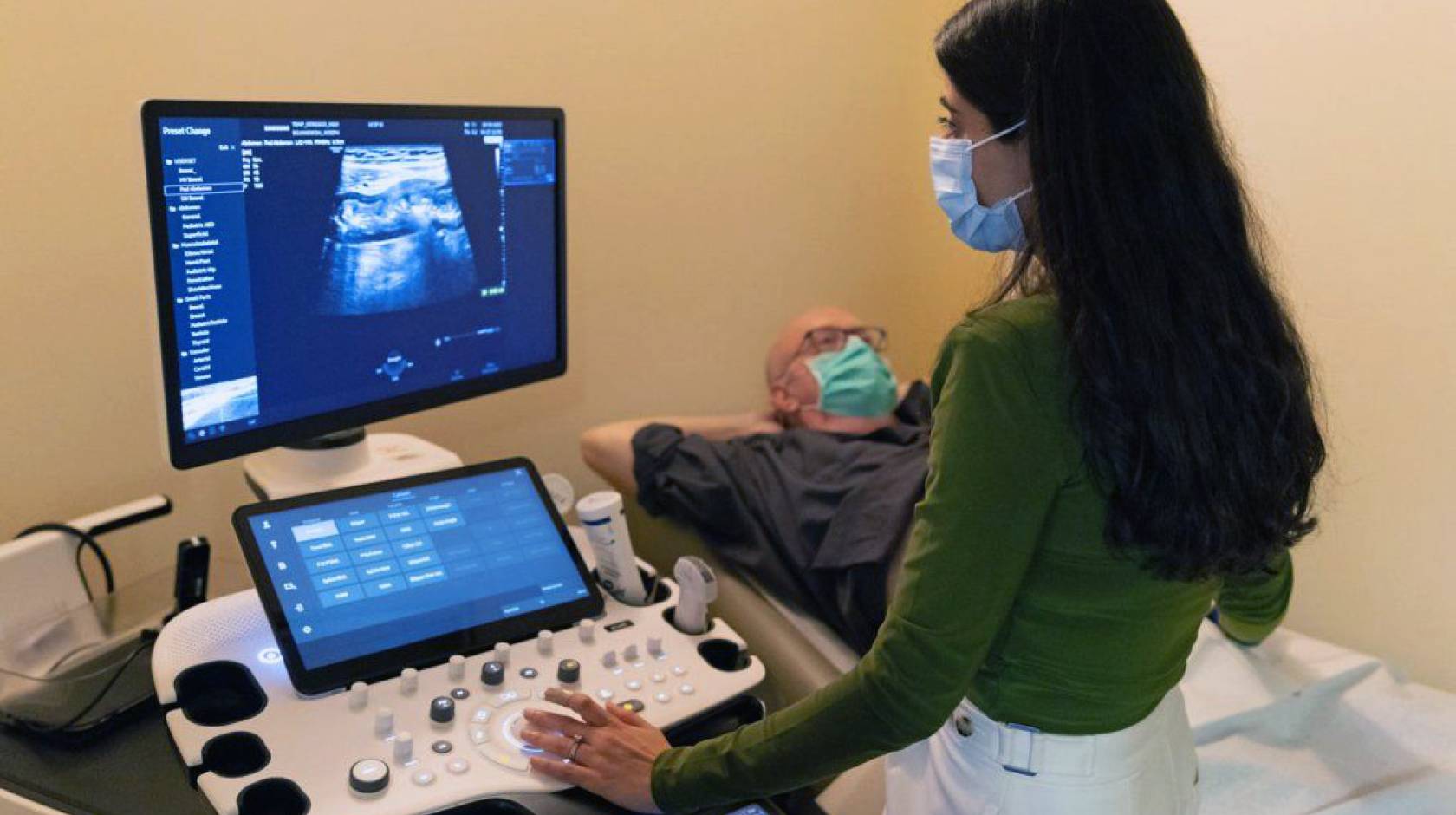
Instead, Bojanowski’s doctor uses intestinal ultrasound to peek at his bowel, which only involves pressing an imaging probe against the outside of his lower abdomen. “The worst it gets is the gel’s a little sticky,” Bojanowski quipped.
As of late March, UCSF Health is officially the first medical facility west of the Mississippi River to house an intestinal ultrasound clinic for adults with IBD. Bojanowski’s gastroenterologist, Rishika Chugh, M.D., UCSF assistant professor of medicine, was motivated to start the clinic out of empathy for patients like Bojanowski.
“An MRI, which we use to examine the small bowel, requires an appointment, fasting, and the use of contrast dye through an IV and/or orally, and colonoscopy requires taking a gallon of laxatives the day before, along with fasting, sedation and an appointment. It’s hard on the patients, who are already suffering,” said Chugh.
“With ultrasound, I can do the exam right then and there during a clinic visit,” Chugh added. “The patient is fully awake and can tell me where it hurts. I can talk them through what I’m doing, and the results are immediate. It’s much less invasive, and my patients love it.”
IBD, which comprises Crohn’s disease and ulcerative colitis, affects 1.3 percent of the U.S. population and accounts for 3 million new diagnoses every year. It is an autoimmune disease and can be treated with 5-aminosalicyclic acids, immunomodulators, corticosteroids, biologics, and in some cases, surgery. Frequently, patients must try many different types of treatment before finding one that works best long-term.
As such, Chugh mainly uses intestinal ultrasound to monitor response to new drugs or changes in treatment. She may also use it to see how the bowel is healing after surgery or to look for disease complications such as an abscess or fistula.
“Ultrasound is really useful here because often we are scheduling four months out for colonoscopies and at least two months out for MRI, and that’s too long of a gap when you are tweaking medications,” Chugh said. “With ultrasound, I can usually see patients in a matter of days.”

Joe Bojanowski and Dr. Rishika Chugh
Only clinic in Northern California
There will still be times when MRI or colonoscopy are needed, she emphasized. “We can’t use ultrasound to screen for cancer – and that’s important to do, because IBD patients are at higher risk for colon cancer,” said Chugh. “Intestinal ultrasound also is limited in terms of evaluating the small bowel and rectum, and of course we can’t do biopsies with this method.”
Getting the clinic off the ground wasn’t easy. While ultrasound is common in Europe and Australia and medical residents are routinely trained in it, the U.S. medical education system doesn’t prioritize it in the same way, said Chugh. As a result, the training here is intensive and expensive.
Currently there are less than two dozen gastroenterologists in the U.S. trained to use intestinal ultrasound for IBD in adults, said Chugh.
“I’m grateful that Uma (Mahadevan, M.D.), who leads the UCSF Crohn’s and Colitis Center, raised philanthropic funds so I could be trained and so we could buy the ultrasound equipment,” said Chugh.
“UCSF is delighted to lead in this important area and be able to offer this service to our IBD patients,” said Mahadevan, professor of medicine. “We are very fortunate to have Dr. Chugh internationally trained and certified to run the program.”