2020 began on an ominous note, as California and the rest of the United States watched from afar while a mysterious respiratory illness made its way through China. Individuals video-conferencing from quarantine, community shutdowns and high-tech contact tracing to find the virus before it could infect someone else: Surely, it would somehow be contained before it happened here?
Yet just a few short months later, the virus overtook the United States, prompting major changes to day-to-day life and causing an unprecedented effort by individuals and institutions to help the sick and mitigate its spread. University of California campuses pivoted to deliver remote instruction to students; across the system the health and research enterprise — which began preparing in the earliest days — immediately took on new projects to try and find a difference-maker.
The good news is, with 2020 coming to a close, relief seems in sight. Multiple vaccines are in development, and distribution is underway. Federal and state governments are drawing up plans to vaccinate hundreds of millions of people in the U.S. by summer. It’s an unprecedented achievement for science, medical research and global cooperation, given vaccines usually take years — or decades — to produce.
The efforts and research of UC campuses and health centers have played a major role in protecting California and exploring viable solutions to stopping the pandemic. Here’s a look at where we started and how far we’ve come with the coronavirus.
Stopping the spread: Testing

UC San Francisco helped to provide COVID-19 testing in the Mission District in April. It is now collaborating to expand testing in several San Francisco neighborhoods.
Today, you can go online and schedule a COVID-19 test with your health care provider, or find free options for COVID-19 testing through local government. But in the earliest days of the pandemic, testing was in extremely short supply.
University of California Health (UCH) began filling that gap in early March, as its CLIA-certified labs developed their own in-house testing for the coronavirus, making UCH one of the first health systems in the country to do so. As the fourth-largest health delivery system in California serving a large number of low-income patients, University of California Health’s capability was significant. In April, UCSF Health announced it was offering free COVID-19 test analysis and results to the public health departments of all 58 California counties.
At the campuses, many researchers applied their expertise to improving testing technologies. 2020 Nobel laureate Jennifer Doudna of UC Berkeley spearheaded a pop-up diagnostics lab at the Innovative Genomics Institute for the campus and members of the surrounding community, including first responders and unhoused people who are especially vulnerable to COVID-19.
“When the pandemic hit, we asked ourselves, ‘What do we as scientists do to address the COVID-19 health emergency?’” Doudna said in June. “That effort has focused on testing. We set up a clinical laboratory, and we are now getting asymptomatic saliva testing going for the UC Berkeley campus.”
The IGI shared its blueprints for starting a pop-up testing lab and methods for surveillance testing in a large campus environment so that similar institutions could learn from their efforts.
In October, scientists at UCLA Health received emergency FDA authorization to begin using a new method of COVID-19 detection utilizing sequencing technology called SwabSeq. The method is capable of testing thousands of samples for coronavirus at the same time, producing accurate, individual results in 12 to 24 hours. The underlying technology of SwabSeq can be applied to any type of sample collection, such as a nasopharyngeal, oropharyngeal or saliva test.
"This is a technological breakthrough that will dramatically increase the amount of COVID-19 testing while reducing the wait time for results and costs," says Dr. John Mazziotta, vice chancellor for UCLA Health Sciences and CEO of UCLA Health.
Stopping the spread: PPE and equipment

Six employees in the costume and scene shops of UC Riverside’s Department of Theatre, Film, and Digital Production sat behind sewing machines, stitching together face masks for their colleagues. Their goal was to make at least 750 masks, which are free for essential UC Riverside employees as a form of supplemental protection.
Personal protective equipment (PPE) and medical supplies were at a premium during the first wave. PPE is now a household name and production has dramatically improved. But in the early days, health care workers were making their own masks, or going on social media to call for donations.
Campuses across the system responded by producing PPE themselves and running donation drives. UC Riverside theater employees sewed face masks for their essential worker colleagues. UC med students, with clinical training paused, reached out to the public and ran donation drives.
Labs across the system also used their technologies to produce PPE: UC Santa Barbara began using 3-D printing to create face shields, while UC San Diego used 3-D printing to retrofit and build ventilators, as did UC Irvine’s School of Medicine.
Stopping the spread: Understanding how the virus works and how to kill it

A team of scientists from UC San Diego (including Nobel laureate Mario Molina) collaborated remotely with colleagues at Caltech and Texas A&M to analyze the transmission pathways of COVID-19. Their study confirmed that face coverings determine the pandemic’s trends and significantly reduce the number of infections.
So much was unknown in the beginning, including how long the SARS-CoV-2 virus could live, and where.
An important early study on the coronavirus and its stability and viability in the air and on surfaces was done by UCLA, noting that the virus could be detected in aerosols (particles suspended in the air) for three hours; up to four hours on copper; up to 24 hours on cardboard; and for up to two to three days on plastic and stainless steel.
While surfaces are no longer believed to be a primary source of transmission, the finding on aerosols was particularly important as an early indicator that tiny particles suspended in air, not necessarily produced by coughing or sneezing, could carry the virus, adding to a growing consensus that prevention required good air ventilation and face coverings.
As early as April, UC Davis asked “how important is speech in transmitting the coronavirus?” which turned out to be a very important question as further research identified airborne transmission as perhaps the most important vector. UC Davis aerosol scientists suggested that normal speech by individuals who are asymptomatic but infected with coronavirus may produce enough aerosolized particles to transmit the infection. These questions built off pre-pandemic research that found that the louder one speaks, the more aerosolized particles are emitted. And some individuals — for reasons that are still not clear — emit up to 10 times as many aerosolized particles as others, making them potential virus “superspreaders.”
Later studies, including one by UC San Diego, confirmed this type of airborne transmission is the dominant route for spreading COVID-19, making masks and face coverings a necessary containment strategy.
UC researchers also began developing a host of new technologies to eliminate the virus on surfaces and disinfect the air inside buildings. Campuses developed novel approaches for killing the virus, with UC Santa Barbara developing a technique using LEDs; UC Irvine focusing on Blu-Ray technologies; and UCLA developing methods using atmospheric plasma sprays.
Stopping the spread: Public health communication and strategies
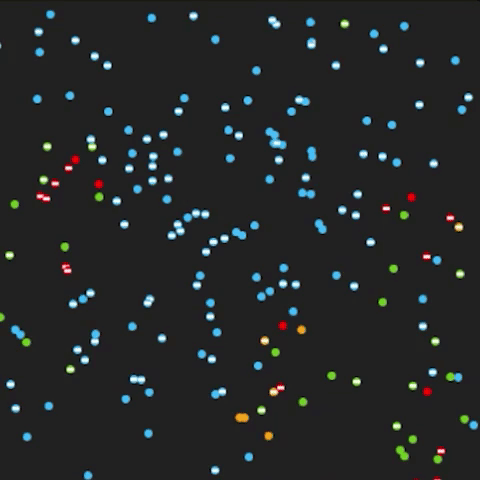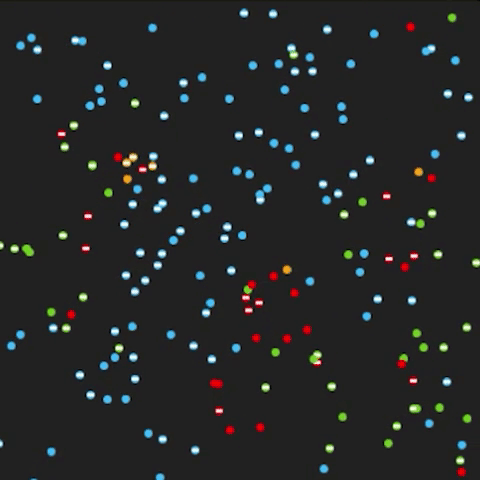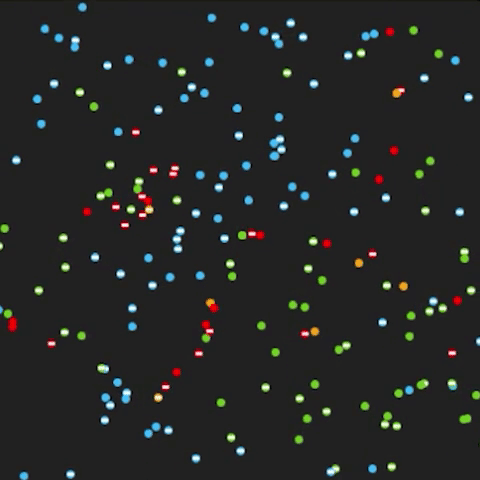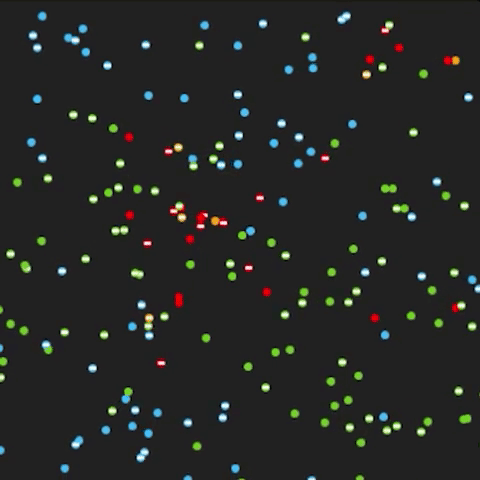
De Kai has created a simulation to show how the transmission of COVID-19 can be slowed by mask wearing. Click the image above to try out the simulator yourself.
Remember when we wondered if, and when, we should even touch our mail? We’ve come a long way in our public health guidance. UC science has explained why masks work; which types of masks work best; and how many people in a population need to mask up to stop the virus from spreading (80-90 percent of the population, according to computer science and engineering professor De Kai at UC Berkeley’s International Computer Science Institute). UCSF has also produced research suggesting wearing a mask or face covering could make you less likely to get seriously ill if you do get infected.
UC scientists also provided important health guidance on the necessity of social distancing and other measures the public can take. UCSF’s Dr. Bob Wachter emerged as an important voice on Twitter with his UCSF COVID Chronicles and appeared everywhere from NPR affiliates to “On Air with Ryan Seacrest” to disseminate information about the virus, and UCLA’s Anne Rimoin providing advice to viewers on “Good Morning America” and other news shows, to name just two.
1/ Covid (@UCSF) Chronicles, Day 259
— Bob Wachter (@Bob_Wachter) December 2, 2020
The vaccine news remains astoundingly positive. Reacting to my upbeat mood, a reporter asked me if there’s anything that keeps me up at night. Aside from the cataclysmic current state of Covid (likely to get worse, I fear), there are a few:
UC San Diego researchers and entrepreneurs developed and led the pilot program for CA Notify, an app that helps reduce the spread of the virus by providing users with a private and anonymous means of sharing information about possible exposures to COVID-19. If exposed, an alert will pop up on your phone to empower you with information to keep your friends, family and community safe. The app is now available to everyone in California, and more than 6 million people have signed up to use it. Until a vaccine has been administered to people across the United States, containment strategies will be vital to saving more lives.
Treating it: Finding new treatments and tapping into existing ones

Searching the massive FDA drug database for potential matches after the first protein targets were found.
A team located at UC San Francisco’s Quantitative Biosciences Institute, QBI, worked around the clock to discover how the coronavirus attacks cells in the hopes of identifying proper therapeutics. But instead of trying to create new drugs based on this information, they first looked to see if there were drugs already available that could fight the coronavirus. In March alone they identified 27 FDA-approved drugs in the hopes of narrowing and speeding up the search.
Also in March, UC Irvine Health and UC San Diego Health launched clinical trials of the antiviral drug remdesivir, originally developed to treat Ebola, which to date is one of the few drugs approved by the FDA for use treating COVID-19. UCLA Health announced its involvement in a National Institutes of Health clinical trial of the same drug in April.
In August, UCSF announced a new possible form of treatment for, and prevention of, COVID-19. Led by UCSF graduate student Michael Schoof, a team of researchers engineered a completely synthetic, production-ready molecule that straitjackets the crucial SARS-CoV-2 machinery that allows the virus to infect cells. In an aerosol formulation they tested, dubbed “AeroNabs” by the researchers, these molecules could be self-administered with a nasal spray or inhaler.
The research team has been in active discussions with commercial partners to ramp up manufacturing and clinical testing of AeroNabs. If these tests are successful, the scientists aim to make AeroNabs widely available as an inexpensive medication to prevent and treat COVID-19.
Treating it: Dealing with long-haul COVID-19

Tackling “long-haul” COVID-19: Mark Avdalovic, director of UC Davis Health’s Post-COVID-19 Clinic, and Namita Sood, pulmonologist.
“We thought it was just a respiratory virus. We were wrong” noted a UCSF news article that explored the emerging science about how COVID-19 affects cells throughout the body, unlike a mere cold or flu. UC scientists documented the loss of smell and taste accompanying infection (and how people misjudge their own loss of smell and taste, a phenomenon noted by UC Merced); other UC researchers pointed to mysterious swelling in children’s toes.
The puzzle of who gets seriously ill, who doesn’t, and why some people’s symptoms persist for months on end remains to be solved. The phenomenon of “long-haul” COVID-19 patients led UC Davis to found a Post-COVID-19 Clinic. Complications from the illness, particularly in terms of how it affects the heart, are the subject of ongoing research across the UC system.
Ending it: Understanding COVID-19 antibodies

A medically trained UC Irvine volunteer collects a blood sample at one of 11 drive-thru antibody testing sites in Orange County.
As scientists sought a vaccine to protect against COVID-19, they focused their attention on antibodies, which can help the body fight off re-infection.
The antibody science of COVID-19, like most aspects related to the illness, has evolved rapidly and grown in sophistication since the pandemic’s early days. In mid-April, UC San Diego launched a pair of serological tests to look for novel coronavirus antibodies — evidence that someone has been infected by the coronavirus, even if they never experienced symptoms. A new test, developed by UC Santa Cruz, can provide complete quantitative results in less than 20 minutes.
Here’s last week's bag of plasma. Such a bag! After the paperwork, it’s as easy as taking a nap. Thanks @arimoin and UCLA. Hanx pic.twitter.com/15WblGiVwe
— Tom Hanks (@tomhanks) April 29, 2020
The research is still developing about how much protection antibodies provide, and for how long, but it is clear that they have utility for those in the midst of fighting the illness. Across the system campuses have encouraged survivors of COVID-19 — including Tom Hanks and Rita Wilson — to donate plasma so it can be used to help seriously ill patients recover. A clinical trial with convalescent plasma at UCLA showed some success in getting patients off ventilators and breathing on their own.
Ending it: The vaccine

A shot of a shot: One of the first vaccinations of a frontline worker at UCSF.
Perhaps no scientific pursuit has seen the focused intensity that has gone into developing a SARS-CoV-2 vaccine. Now, in defiance of projections that it might take years, two have been approved for use in the United States, having already gone through successful clinical trials.
UCH has participated in all of the major vaccine trials, with its staff and faculty rolling up their sleeves for these experimental therapies.
Kristen Choi, a UCLA assistant professor of nursing who participated in Pfizer’s vaccine trial, said that physicians and other health care professionals now need to help their patients have trust in the vaccine and its safety.
“They will need to explain that fatigue, headache, chills, muscle pain, and fever are normal, reactogenic immune responses and a sign that the vaccine is working, despite the unfortunate similarities with the disease’s symptoms.”
While it cannot be known whether or not she received the vaccine or a placebo, her experience with flu-shot like side effects is an important cautionary tale for the next, long-awaited step of COVID-19 public health outreach: what to expect when you receive a COVID-19 vaccine.